By James Simons–
An NHS office manager has revealed her personal, life-saving experience with a new artificial intelligence (AI) skin cancer screening tool she helped introduce at her workplace. Lynsey Robertson, who works at a GP surgery in Preston, Lancashire, oversaw the implementation of the cutting-edge technology designed to speed up the diagnosis of potential melanomas.

Lynsey Robertson found out she had a deadly form of melanoma after trying out new technology at her office (Supplied)
Curiosity led her to test the system on a mole she had mostly disregarded for years, a decision that proved to be unexpectedly critical. Within hours, the new AI system flagged the lesion as high-risk, initiating a rapid referral that confirmed the presence of an aggressive malignant melanoma.
The entire experience profoundly affected Mrs. Robertson. She immediately realised that if she had not decided to try the innovative technology at that moment, the outcome could have been drastically different. Her quick diagnosis and successful surgery highlight the immediate and tangible benefits of the ongoing AI screening rollout across the health service. She is now urging people everywhere not to ignore changes in their skin.
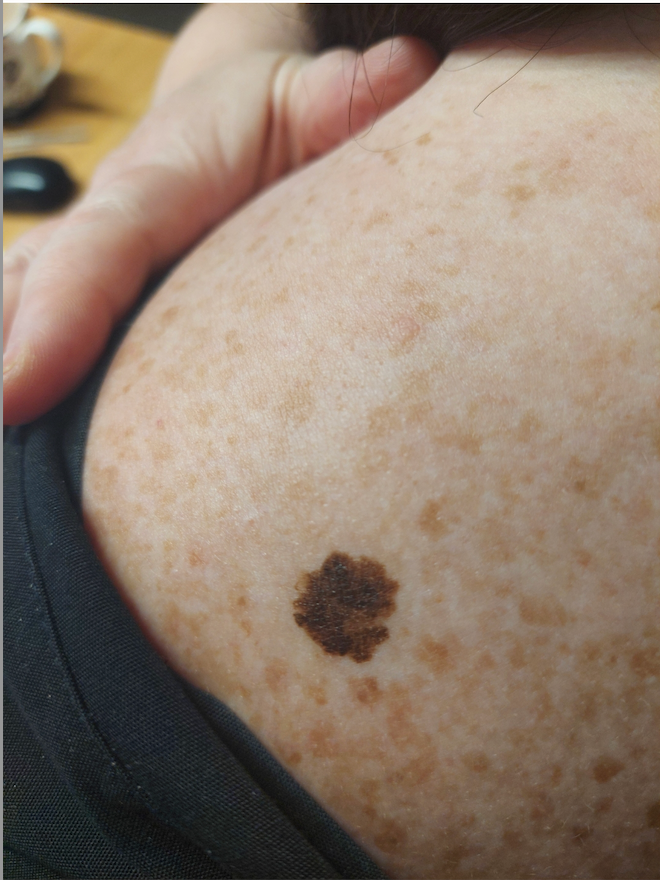
Lynsey Robertson ignored her mole for years. Supplied
The Power of the AI Screening Rollout
Mrs. Robertson’s story provides a powerful case study for the efficiency and accuracy of AI in medicine. The technology, known as DERM (Deep Ensemble for Recognition of Malignancy) and developed by Skin Analytics, uses a sophisticated algorithm to analyse high-resolution images of skin lesions.
Clinicians use a smartphone with a specialised magnifying lens attachment to capture the necessary images. The system then rapidly compares the lesion’s characteristics against a vast database of skin conditions to determine its risk level.
.jpeg)
Skin Analytics developed the Deep Ensemble for Recognition of Malignancy technology. Skin Analytics
The AI’s ability to triage cases quickly aims to alleviate mounting pressure on dermatology departments. Experts believe the widespread adoption of the AI screening rollout can significantly reduce waiting times for specialist appointments.
The technology boasts a remarkable 99.9% accuracy rate in ruling out melanoma, giving patients peace of mind quickly when results are benign. This autonomous capability allows human dermatologists to focus their precious time on genuinely urgent cancer cases, streamlining the entire diagnostic pathway for the National Health Service.
A Call for Greater AI Integration in Patient Care
Mrs. Robertson, 46, acknowledged that her mole did not cause any pain and she had always assumed it was not serious enough to trouble a doctor. Her hesitation is common, demonstrating a barrier that the current AI system successfully bypasses.
The technology’s ability to provide an objective, rapid assessment in a primary care setting eliminates the common fear of “wasting the GP’s time.” She underwent minor surgery quickly to remove the mole and a subsequent procedure to ensure the removal of all cancerous cells.
The UK’s National Institute for Health and Care Excellence (NICE) has conditionally recommended the use of this AI technology in the NHS for a three-year evidence-gathering period and has assessed more than 170,000 NHS patients since the year 2020, reflecting its promising results in maintaining diagnostic accuracy while cutting wait times.
This positive personal outcome underscores the importance of technological innovation in public health. Experts suggest that a wider AI screening rollout could ultimately save thousands of lives annually through earlier detection.

The NHS employs AI in hospitals and clinics. King’s College London/PA Wire
As healthcare systems continue to embrace digital transformation, the success of AI screening programmes like this one sets a precedent for future advancements in medical technology. Integrating AI into routine patient care not only enhances clinical efficiency but can also help address disparities in access to specialist diagnostics, particularly in rural or underserved areas.
Ongoing collaboration between clinicians, technologists, and policymakers will be vital to ensuring that such innovations are implemented safely, ethically, and to the greatest benefit of patients across the country.








