By James Simons-
CHANDIGARH, India — In a far-reaching judgment with profound implications for healthcare across the subcontinent, the Punjab and Haryana High Court recently made a resounding declaration: a legible medical prescription constitutes a Legible Medical Prescription Fundamental Right.

Pic: iStock
Justice Jasgurpreet Singh Puri, delivering the landmark order, directly linked the right to a clear prescription to the fundamental Right to Life and Personal Liberty guaranteed by Article 21 of the Indian Constitution.

Justice Jasgurpreet Singh Puri
This ruling, which followed the court’s dismay over an “incomprehensible” medical document, mandates a systemic shift in how medical professionals communicate treatment and diagnosis.
The court has effectively created a two-pronged approach to solving the endemic problem of illegible medical handwriting.
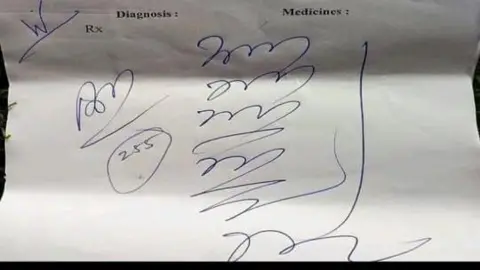
Chilukuri Paramathama: An illegible prescription by an Indian doctor in Madhya Pradesh state last year went viral. BBC
First, until the digitisation is complete, Justice Puri directed that all doctors in Punjab, Haryana, and the Union Territory of Chandigarh must write their prescriptions and diagnosis notes clearly in capital letters.
Second, and more importantly, the order sets a firm two-year deadline for the government to fully implement computerised or typed prescriptions, with provisions for financial assistance to clinical establishments where needed.
This is not simply a call for tidier notes; it is a constitutional imperative for patient safety, recognising that a Legible Medical Prescription Fundamental Right is non-negotiable.
The catalyst for this judicial intervention was not a medical negligence case, but an unrelated anticipatory bail plea concerning allegations of cheating, forgery, and sexual exploitation.
While examining the evidence, Justice Puri reviewed the medico-legal report prepared by a government doctor who had examined the complainant. That report was so poorly written that it was rendered useless.
The judge was visibly shocked, observing in his order, “It shook the conscience of this court as not even a word or a letter was legible.” This moment of judicial frustration highlighted a systemic failure that has long plagued India’s healthcare system.
The court noted the shocking paradox of illegible paper prescriptions persisting in an era of unprecedented technological advancement.
“It is very surprising and shocking to note that in this era of technology and accessibility of computers, the notes on the medical history and on the prescriptions by the Government doctors are still written by hand,” the judgment stated, adding that these notes “cannot be read by anybody except perhaps some chemists.”
Therefore, enforcing a Legible Medical Prescription Fundamental Right became an urgent matter of public interest, compelling the court to intervene decisively.
Training and Digitisation
In a key directive aimed at long-term systemic change, the court requested the National Medical Commission (NMC) to introduce and integrate the importance of clear, legible handwriting into the curriculum of all medical colleges across the nation.
This proposal acknowledges that improving penmanship must begin at the educational foundation of the medical profession.
Simultaneously, the two-year deadline for rolling out digital prescriptions will accelerate the national push towards Electronic Health Records (EHRs) and e-prescribing systems.
Institutions like the Post Graduate Institute of Medical Education & Research (PGIMER) in Chandigarh have already committed to implementing their e-prescription module within this timeframe, setting a precedent for public health infrastructure.
Dr Dilip Bhanushali, President of the Indian Medical Association (IMA), which represents over 330,000 doctors, acknowledged the association’s willingness to collaborate on a solution.
He pointed out the practical challenges, stating that while urban centres are increasingly adopting digital prescriptions, implementation remains difficult in overcrowded government hospitals, particularly in rural areas and smaller towns. “A doctor who sees seven patients a day can do it, but if you see 70 patients a day, you can’t do it,” he argued, linking poor handwriting to the immense pressure and patient load faced by practitioners.
However, he reaffirmed the IMA’s recommendation that members should “write prescriptions in bold letters that should be readable to both patients and chemists.”
Experts consistently warn that a prescription leaving room for misinterpretation can carry devastating, even tragic, consequences for the patient.
The problem is not merely an issue of aesthetics or convenience; it is a matter of life and death, reinforcing the necessity of a Legible Medical Prescription Fundamental Right.
Globally, the risks have been quantified. For example, a 1999 report by the U.S. Institute of Medicine (IoM) estimated that medical errors cause at least 44,000 preventable deaths annually in the United States, with a staggering 7,000 of those deaths directly attributable to sloppy handwriting. These figures highlight the international scope of the crisis.
In a recent and illustrative case in Scotland, a woman suffered chemical injuries after a pharmacist mistakenly dispensed erectile dysfunction cream instead of the eye ointment she had been prescribed.
In the UK, health authorities have admitted that “drug errors caused appalling levels of harm and deaths,” suggesting that the “roll out of electronic prescribing systems across more hospitals could reduce errors by 50%.”
While India lacks similarly robust, nationwide data on harm caused by poor handwriting, anecdotal evidence and high-profile incidents underscore the danger.
One widely reported case involved a woman who experienced severe convulsions after inadvertently taking a medicine intended for diabetes, which had a name similar to a prescribed analgesic.
Such instances confirm that the misreading of prescriptions has resulted in numerous health emergencies and avoidable fatalities across the world’s second-most populous country.
This situation demands a firm resolution, confirming that the court’s declaration of a Legible Medical Prescription Fundamental Right is long overdue.
The campaign for legible prescriptions gained significant legal momentum a decade ago.
In 2014, Chilukuri Paramathama, a pharmacist running a shop in Nalgonda city in the southern Indian state of Telangana, filed a public interest petition in the high court in Hyderabad. His action was spurred by news reports concerning the death of a three-year-old child in Noida city, who died after a wrong injection was administered for a fever. This tragedy epitomised the risks inherent in ambiguous medical communication.
Mr. Chilukuri’s dedicated campaign, which sought a complete ban on handwritten prescriptions, partially achieved its objective in 2016. At that time, the Medical Council of India (MCI) issued an order mandating that “every physician should prescribe drugs with generic names legibly and preferably in capital letters.” Despite this regulatory move, pharmacists like Mr. Chilukuri and his colleagues report that poorly-written prescriptions continue to arrive at their counters.
Ravindra Khandelwal, the CEO of Dhanwantary, a well-known pharmacy chain in Kolkata with 28 branches serving over 4,000 customers daily, affirmed this ongoing challenge. He noted that while metropolitan areas show a shift towards printed forms, most prescriptions in suburban and rural areas are still handwritten, often “border[ing] on the illegible.”
Pharmacists frequently become the last line of defence against a fatal error. Mr. Khandelwal’s staff, who possess considerable experience, can often decipher most of the scrawled notes. “Even so, sometimes we have to call the doctors because it’s very important for us to dispense the correct medicine,” he explained, illustrating the time-consuming and hazardous interpretation process.
The persistent nature of the problem, despite the 2016 MCI order and a 2020 parliamentary statement by junior health minister Ashwini Kumar Choubey assuring disciplinary action against non-compliant doctors, underscores the significance of the latest judicial mandate.
By constitutionalising the issue, the Punjab and Haryana High Court has elevated the right to a clear prescription above mere regulatory guidelines, solidifying the Legible Medical Prescription Fundamental Right for every Indian citizen.
Previous calls for reform from other High Courts, including those in Odisha and Allahabad, which flagged “zigzag style of writing” and “shabby handwriting,” demonstrate that this is a nationwide systemic problem requiring a high-level, decisive solution.
The court’s final order marks a crucial turning point, setting a clear trajectory towards the mandatory digitisation of medical records and prescriptions.
This shift promises not only to reduce prescription errors and save lives but also to enhance patient autonomy, allowing individuals to clearly understand their medical status and treatment plan.




